Clinical Pearls – 2017
The continuing saga of insulin resistance and fat – December 10th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
December 10th, 2017
The continuing saga of insulin resistance and fat
I’m continuing to review the studies I shared with you a couple of weeks ago, with the intention for writing a comprehensive blog post in January. This week, I chose to analyze this article:
Lipid overload and overflow: metabolic trauma and the metabolic syndrome
https://www.ncbi.nlm.nih.gov/pubmed/14580758 – this is the abstract. I purchased the full study, and it’s HERE but don’t post this or publish it anywhere as it’s just for NEPT members.
This article takes an interesting perspective on the etiology of insulin resistance, and it’s relationship to lipogenesis.
The author does not address dietary fat as a cause of insulin resistance; rather he addresses “overnutrition” and “underexertion” He makes 3 very good points:
- Insulin resistance of obesity triggers insulin-stimulated lipogenesis – meaning that resistance to insulin uptake of glucose triggers the creation of fat.
- Resistance to the uptake of surplus glucose might be a defense against lipid overaccumulation in lean tissues
- The underlying cause of the metabolic syndrome is leptin-resistance.
According to this article, insulin induces expression of the enzymes of lipogenesis through upregulation of the lipogenic transcription factor, SREBP-1c.
He observes that when obesity is induced in normal rats by overfeeding, a diet of 60% fat, most of the excess fat (96%) is deposited in adipose tissue. In leptin resistant rats, even on a low fat diet, much of the excess is deposited in non-adipose tissue.
So what is the true cause of insulin resistance? It would appear to related to consuming more calories that are burned. Nothing in this article differentiates between fat calories and sugar calories.
Insulin Resistance – November 26th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
November 26th, 2017
I reviewed the following article on insulin resistance and wrote a few words about it here – lets discuss on the net site. I’d love to hear your perspective.
Recall from last week, that these articles were presented to me as evidence that fat, not sugar, is the primary cause of insulin resistance.
This article discusses the impact of excess fatty acids on insulin resistance, not a high fat diet, calorically sufficient diet. Increased free fatty acids are the result of excess calories, regardless of source, as the body converts sugar into fatty acids for storage.
In fact, the author concludes that excess calories, regardless of source, will cause insulin resistance. Here are paraphrases from the last 2 paragraphs.
“…it was reported that a 20% higher energy intake was associated with a 2.4-fold higher risk of developing diabetes. This effect appeared to be due primarily to the fact that higher energy intake was associated tightly with higher body fatness. This reinforces the robust link between excess energy intake, insulin resistance, and the development of diabetes.
In summary, a variety of lines of evidence suggest that insulin resistance, in large part, is a cellular defense mechanism against energy excess. Cellular energy excess is caused primarily by the chronic consumption of energy in excess of what is expended. Fat tissue can mop up the excess energy for a while, but if the excess is chronic and fat tissue enlarges (particularly abdominal fat), other tissues will be exposed to progressively more energy (fatty acids and glucose), and cells will act to protect themselves by reducing insulin sensitivity.”
Micronutrients – November 17th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
November 17th, 2017
One of our IRSPT students asked me to comment on the impact of saturated fats on insulin resistance. There are people who claim it’s not sugar that causes insulin resistance , its fat, especially saturated fat.
I think the answer is a bit more complex than people make it out to be. Oxidized fats, poor quality fates, and too much omega 6 and saturated fats certainly have an impact.
I plan to write more in-depth article about this, and to comment on the articles below .
I’d love your opinion about these
Does Increasing circulating free fatty acids in humans rapidly induces insulin resistance ?
What Causes Insulin Resistance? Part I
http://wholehealthsource.blogspot.my/…/what-causes-insulin-…
Insulin resistance is a cellular antioxidant defense mechanism
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2764908/
Lipid overload and overflow: metabolic trauma and the metabolic syndrome
https://www.ncbi.nlm.nih.gov/pubmed/14580758
Effect of fatty acids on glucose production and utilization in man
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC370462/
Effects of fat on insulin-stimulated carbohydrate metabolism in normal men.
https://www.ncbi.nlm.nih.gov/pubmed/1885781
Interaction between glucose and free fatty acid metabolism in human skeletal muscle.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC293539/
Effects of free fatty acids on glucose transport and IRS-1–associated phosphatidylinositol 3-kinase activity: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC407880/
Dose-response effect of elevated plasma free fatty acid on insulin signaling.
https://www.ncbi.nlm.nih.gov/pubmed/15919784
Overnight lowering of free fatty acids with Acipimox improves insulin resistance and glucose tolerance in obese diabetic and nondiabetic subjects.
https://www.ncbi.nlm.nih.gov/pubmed/10480616
Micronutrients & Insulin Resistance – November 12th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
November 12th, 2017
Our clinical pearl this week is on the importance of micronutrients in managing insulin resistance and diabetes. Take a look at these recent articles resistance:
https://www.eurekalert.org/pub_releases/2017-11/ru-rus110717.php
I look forward to connecting soon
Naturopaths – October 29nd, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
October 29nd, 2017
Have you ever wondered about the so-called stones that are released during a liver – gallbladder cleanse? I call them “Bile Balls” because they are green and squishy. And there are a lot of skeptics, among naturopaths and the public, about their constituents.
Here’s an FAQ about the flush, from Andreas Moritz
The mayo clinic warns against them, but doesn’t really say much
And so does this plant-based site
http://plantbasedu.com/the-liver-and-gallbladder-flush-is-dangerous-and-a-scam/
So what’s the truth? I suggest you check it out for yourself. Personally i don’t recommend people do them without the guidance of someone with experience – someone who can discern whether you are a good candidate.
I suggest you reach out to Jane, and participate in her cleanse. It’s gentle, effective and from what I’ve seen, people feel a renewed sense of vitality afterward.
So whether the “stones” are really stoned – or they are congealed bile and fat, it really doesn’t matter , does it?
Jane Gyette did a facebook live event on Thursday-. She interviewed a sonographer who took videos of an ultrasound scan during a cleanse.
I’ve done jane’s cleanse a few times and it’s amazing.
Insulin Resistance in the News – October 22nd, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
October 22nd, 2017
Insulin Resistance in the News
I subscribe to google alerts for the term insulin resistance. Some of the articles flagged are good, some mediocre. It’s a good idea to subscribe to topics you’re interested in, to keep up with the latest. This can give you ideas for blog posts, Facebook posts and other communications with your prospective clients. Here are a few I found interesting.
We talk about the underlying, insidious causes of insulin resistance related to processed food, lack of movement, sleep deprivation, stress and poor timing of meals. A recent article demonstrates the risk related to exposure to to third-hand smoke – on clothing, hair, and clothing. http://www.clinsci.org/content/131/19/2409
Another talks about evidence that excess salt intake can contribute to the development of type 2 diabetes and LADA (latent autoimmune diabetes in adulthood). http://www.hindustantimes.com/fitness/worried-about-getting-diabetes-cut-down-on-chips-and-other-salty-foods/story-3vub3yFXVzXjLNzQertKOL.html
And finally one on the link between eating red meat and type 2 diabetes. Here’s to a vegetable based diet with limited meat.
http://www.mdmag.com/medical-news/study-red-meat-and-heme-iron-linked-to-type-2-diabetes
Bone Broth – Pros and Cons – October 15th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
October 8th, 2017
Bone Broth – Pros and Cons
There is a big push for everyone to consume bone broth on a regular basis. A discussion about this came about on our Facebook group, so I thought it would make a good clinical pearl, and food for thought as our clients will ask about it.
It’s touted as the best (and by some the only) way to heal leaky gut. It’s also applauded for tightening skin, making you look younger and getting rid of wrinkles. The traditional use for collagen supplementation is for healing from injuries – sprains, strains, and fractures, as well as strengthening cartilage.
The downside of bone broth consumption is increased exposure to toxins, and heavy metals, in particular lead.
I suggest you research and make a decision for yourself, then work with each client as an individual and help them to decide if it’s a good option for them.
The original study on lead in Bone Broth:
https://www.ncbi.nlm.nih.gov/pubmed/23375414
Chris Kresser’s rebuttal – I don’t buy him using the FDA’s “safe range” as an argument. If you already have lead exposure and accumulation, that doesn’t cut it for me. Plus who trusts the FDA for safe ranges?
https://chriskresser.com/bone-broth-and-lead-toxicity-should-you-be-concerned/
A blogger’s argument for believing the science, not the paleo writers rebuttals
http://tamararubin.com/2017/03/bone_broth/
Mark Sissen’s opinion:
https://www.marksdailyapple.com/lead-in-bone-broth-cooked-and-cooled-potatoes-and-stress-strategies/
Dr. Michael Gregor – he is very opposed to animal products of any kind, including broth, and he cites science that supports his beliefs
https://nutritionfacts.org/video/lead-contamination-bone-broth/
When it comes down to it, there are pluses and negatives – and you have to decide for yourself, and guide your clients to do the same – and help them to see if they are super sensitive and already have heavy metal exposure, they may want to get the benefits from the nutrients.
Here’s an article that outlines the nutrients in bone broth:
https://fearlesseating.net/when-bone-broth-is-bad-for-you/
Plus there are “No Bone” recipes designed to provide the same or similar benefits:
- http://www.organicauthority.com/a-vegan-bone-broth-recipe/
- http://www.organicauthority.com/a-vegan-bone-broth-recipe/Alternative
- https://www.yogajournal.com/practice/ask-expert-vegetarian-bone-broth
Just remember, the nutrients and collagen in bone broth do not get absorbed and used whole. They are broken down to their amino acid and nutrient constituents then the body used the nutrients to build collagen. So the original source doesn’t really matter – if all the nutrients needed to make collagen are present.
My typical approach for myself is “When in doubt, leave it out” and I opt for plant versions of my nutrients.
DUTCH test – October 8th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
October 8th, 2017
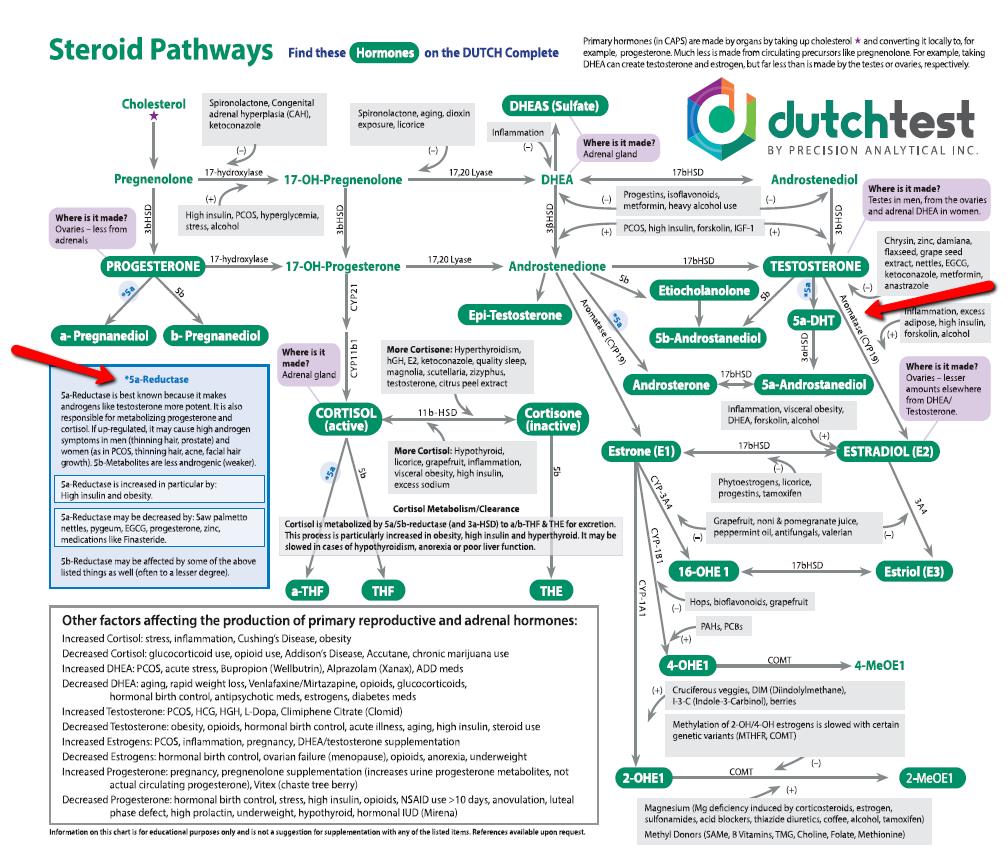
When Testosterone and DHEA Supplementation may NOT a good idea: Exploring Aromatase and 5-Alpha Reductase
What are your thoughts when a male client tells you that his doctor prescribed testosterone – bio-identical – because his blood test was low?
Sounds reasonable and pretty harmless , UNLESS…
His aromatase and 5-alpha reductase activity are in excess.
Aromatase converts estrogen to testosterone, and 5-alpha reductase converts testosterone to DHT (di-hydro testosterone), a potent and potentially carcinogenic form of testosterone.
In the presence of excess aromatase, males can become estrogen dominant – putting them at risk of hormonal cancers and moobs. That’s right, male boobs, common in older men, is often a sign of excess aromatase activity.
I bet you’ll never see those jiggly breasted men at the beach the same again.
DHT elevation can lead to prostate issues.
So what’s the solution? Aromatase inhibitors and 5-alpha reductase inhibitors.
There are pharmaceutical versions of both, but there are also natural ones too – herbs, foods adn nutrients.
Here’s a chart i LOVE! Its from the DUTCH test. At first glance it might seem overwhelming, but trust me – it will become your friend. You can pretty much look up any step in the steroid pathways and see what co-factors promote eahc step. I’ve pointed to aromatase and 5-alpha reductase.
We’ll be going into much more detail about this is an upcoming Mastery module, and we visit it on many lab and case study calls.
Below the picture Iv’e given you a table of aromatase and 5-alpha reductase inhibitors. There are overlaps.
Happy hormone sleuthing!!
| Aromatase Inhibitors | 5-alpha Reductase Inhibitors |
| Nettles
Zinc Damiana Grape seed extract EGCG (from green tea) Collards Cacao Isoflavones and flavonoids Cruciferous vegetables Nuts and seeds Coconut ‘Garlic and onions Herbs such as oregano, thyme, rosemary, sage and turmeric |
Nettles
Zinc Pygeum Saw palmetto EGCG (from green tea) Progesterone Asthaxanthin Reishi Cactus flower Alkaline diet |
In addition to the inhibitors, you need to look at factors that increase the activity of these enzymes, most notably excess insulin, anti-fungal medications, alcohol, a variety of medications and excess adipose tissue.
References:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3074486/
http://drjockers.com/the-7-best-aromatase-inhibiting-foods-and-herbs/
http://www.greenmedinfo.com/pharmacological-action/5-alpha-reductase-inhibitor
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1502352/
DUTCH test – September 24th, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
September 24th, 2017
On our coaching call on Thursday, I reviewed a very interesting DUTCH test. The client was a 59-year-old woman with a history of difficulty reducing weight – in spite of major diet changes and an intensive exercise regime.
She had decent low-end-to-normal range – cortisol and DHEA findings, low progesterone, and completely tanked estrogen and testosterone.
What we discovered was over-activity of the reductase enzymes that convert androstenedione to etiocholanolone and androsterone. What this means is that instead of converting DHEA to testosterone, she had a buildup of these metabolytes and low testosterone.
In particular, there was over-activity of the 5-beta-reductase enzyme rather than 5-alpha reductase over-activity, which is more common. I did a little bit of digging and found that it revealed that a potential cause of this is low bile flow, indicative of a sluggish liver/gall bladder.
Here are a couple of references I found.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1383127
https://www.ncbi.nlm.nih.gov/pubmed/19515843
http://www.endocrine-abstracts.org/ea/0007/ea0007p204.htm
https://en.wikipedia.org/wiki/5%CE%B1-Reductase_inhib
To learn more watch the recording of Thursday’s call.
Click the link to review the DUTCH Test report.
Dr. Valter Longo – September 17, 2017
Nutritional Endocrinology Practitioner Training (NEPT)
Clinical Pearl
September 17th, 2017
I’ve been researching lately about fasting mimicking diets. I pre-ordered a book by an Italian researcher, Dr. Valter Longo. The idea is that fasting has some amazing healing benefits when it comes to weight, blood sugar, cancer prevention and reversal, breaking down of cardiovascular plaques and much more.
The problem with fasting is, for obvious reasons, it’s not sustainable :). The other problem is that most people are not willing to try it, even for a day or two, and many can’t for medical reasons.
So, Dr. Longo and colleagues came up with a solution that shows promise – the Fasting Mimicking Diet.
The research is in it’s early stages, but shows great promise. Dr. Joel Kahn, an integrative, plant based cardiologist reports having dropped 40 lbs and experiencing major health benefits over several months. And he’s reporting good results with patients.
The general idea is to eat a plant-only, low carb and protein, relatively high fat (by % of calories) diet consisting of 900-1100 calories for 5 days a month.The rest of the month you eat “normally”.
They’ve developed a packaged meal replacement program that can be used for folks in a hurry, travelling or not fond of food prep.
I haven’t done this myself – but I am considering ordering the packaged meals and trying to create my own version as well. I know that many of our clients would love the convenience of a packaged meal kit.
Here’s a few resources for learning more:
Longevity Diet by Dr. Valter Longo (pre-ordered) – English version due this fall:
Fasting Mimicking Diet by Odelia Rosie: I ordered this on kindle – will report back:
Prolon Fasting Mimicking Diet:
https://prolonfmd.com/fasting-mimicking-diet/
This Doctor Tried A Fasting Mimicking Diet For 2 Months: Here’s What Happened
How a Fasting-Mimicking Diet Can Help You Live Longer
http://articles.mercola.com/sites/articles/archive/2017/07/23/fasting-mimicking-diet.aspx
I Tried a Fasting Mimicking Diet
http://liveanddiet.com/2017/07/fasting-mimicking-diet.html
Mimicking the Fasting Mimicking Diet – My 5-Day Experiment
https://www.quantifiedbob.com/2016/04/fasting-mimicking-diet/
Fasting Mimicking Diet Do-It-Yourself Guide
http://foreverfreefrom.com/fasting-mimicking-diet-guide/
I tried the fasting-mimicking diet and would 100 percent do it again
http://coach.nine.com.au/2017/06/09/10/26/fasting-mimicking-diet-prolon